How Did I Get Arthritis and Is It Curable?
This morning Professor James from the local community college came to my office complaining of knee pain. His knee was not quite right since taking a hard-hit playing football decades ago. He had knee surgery back in the day, and since then was able to play golf and live a regular life – until fairly recently, that is. Over the past several years he often felt pain and grinding. He told me his knee now felt crooked and he just doesn’t trust it not to give out on him. When I looked at his X-rays, it was obvious he had advanced arthritis.
The typical questions I hear following a diagnosis are:
What exactly is arthritis?
How did that happen?
Is there a way to fix the problem without surgery or is a joint replacement the only option?
What Exactly Is Arthritis?
Arthritis is the progressive degeneration of the cartilage between joints. While there are different kinds of joints throughout the body that are supported by ligaments and muscles, they all function to move our arms and legs. The cartilage present at the end of the bones can wear out or accrue damage over time. At times ligaments, tendons, meniscus, or other important structures wear out in the process as well.
How Does Arthritis Happen?
Multiple factors can cause cartilage damage and arthritis. Some people are born with a genetic predisposition or a variation of their anatomy that causes more stress on a joint than the average person. Others may wear their joints out faster because they carry extra weight, work heavy labor jobs, or play intense contact sports like football. Sports injuries or other accidents can jumpstart the process even if the initial injury is no longer an issue. Whatever the cause or underlying condition, the cartilage wear adds up over time.
When the Cartilage Wears Out
Healthy cartilage is a smooth, white, resilient rubber-like padding that absorbs stress and protects the ends of long bones at the joints and nerves. Cartilage damage may start as a small tear, chip, or crack, but eventually becomes a large defect such that bone rubs on bone. This defect causes pain, inflammation, bone spur formation, stiffness, grinding, instability, and even deformity of the limb.
Arthritis is often diagnosed with the assistance of X-rays; we can see when joint spaces become narrower, indirectly revealing cartilage loss. Alternatively, we can diagnose arthritis with an MRI which shows the injury in higher definition. With minimal and localized cartilage loss, it may be possible to transplant cartilage from one part of a joint to another.
Our bodies are not able to naturally repair arthritis or damage within our joints because it has no blood vessels. This means oxygenated red blood cells can’t reach the damaged tissue.
But that doesn’t mean there is no hope.
How to Treat Arthritis
Although there’s no cure for arthritis, treatments in recent years improved greatly. Several viable treatment options exist for arthritis before you need to consider surgery.
Read on to find answers to the question, “How to treat arthritis?”.
Weight loss
Losing excess weight takes stress away from joint movement with each step and both relieves pain and slows down the progression of arthritis. In fact, one pound of weight loss actually takes 4 pounds of stress off the knee during each step. Sometimes, losing weight is an essential step before surgery becomes a consideration; the risk of complications after surgery is higher with obesity.
Physical therapy
Physical therapy helps support joints starting to wear out by improving flexibility and strengthening muscles.
Braces
In certain cases where a knee becomes bow-legged or knock-kneed, a brace can help correct the deformity.
Anti-inflammatory Meds
Anti-inflammatory medications like Ibuprofen, Aleve, Meloxicam, or Celebrex can help with pain caused by arthritis inflammation. Additionally, there are joint health supplements worth considering whether you are experiencing symptoms of arthritis or choosing to take precautionary steps to minimize its impact as you age.
Injections
Injections are another option and come in several different varieties.
Steroids or cortisone
Steroids or cortisone-type medications are my go-to for a first-time injection. They are inexpensive, relatively low-risk, and covered by insurance.
Hyaluronic acid
If steroids or cortisone medications are not appropriate for a patient or don’t work, I consider injections with a chemical called hyaluronic acid, also known as the “rooster comb” injection, Hyaluronic acid was originally harvested from roosters, but is now made synthetically in a lab. It mimics a naturally occurring chemical thought to possibly lubricate the joint, and decrease inflammation and pain.
Platelet-rich plasma
A newer and more expensive option is platelet-rich plasma or PRP. This procedure involves taking the patient’s blood and harvesting the healing factors, then reinjecting it into a specific area or joint.
Stem cells
The last option is stem cells. Advocates of stem cell treatments hypothesize stem cells can transform to accommodate a certain need when placed in a certain environment. For example, stem cells placed near damaged cartilage may develop into cartilage tissue. While there is a lot of promise associated with this therapy, at this point there is no proven benefit, and the cost is often prohibitive.
X-rays before and after knee replacement
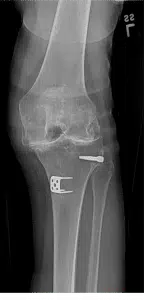
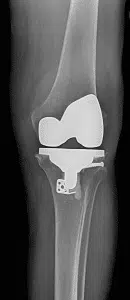
When Is It Time to Consider Surgery?
For many people, arthritis is an annoyance that flares up now and again. Often, we successfully treat the condition with one of the methods above. Sometimes, though, the pain won’t subside as it did in the past, or the instability, deformity, and grinding increasingly get worse. Once patients begin to run out of options or have to cut back on activities important to their lifestyle, surgery becomes a part of the conversation.
Several viable joint replacement options exist for fingers, elbows, shoulders, hips, knees, ankles, and even toes. The rehab process and implant quality has improved in recent years and patients now get joint replacements earlier in life. Implant longevity is hard to predict, and like tire wear on a car, how long a joint lasts depends on how it is used. Generally speaking, there is about a 0.5-1% chance each year a patient will need another surgery on a replaced joint. That means even 80% of joint replacements that are 20 years old are still in place and working decades later.
Surgery is a big decision, but when it’s the right time, it can be life changing.
Professor James tried injections, therapy, braces, weight loss, and anti-inflammatory pills, but still, his walks around campus became more difficult, and stairs increasingly dangerous. It was therefore time to consider surgery. He decided to have knee replacement surgery over the holiday break. He was back to teaching by the time school was back in session – with a straight knee and a newfound endurance!
The Bottom Line
If arthritis bothers you, be encouraged that excellent options are available before surgery. But if it turns out you do need a joint replacement, don’t despair. The current technology is very good and continues to improve all the time.
There are always new techniques to keep arthritis from holding you back!
About the Author: Adam Wright, M.D.

Adam Wright, M.D. is a fellowship-trained orthopedic surgeon specializing in both routine and complex joint replacement of the hip and knee at the Plano Orthopedic & Sports Medicine Center in Plano, Texas. He is proficient in emerging and innovative techniques in primary and revision arthroplasty including minimally invasive surgery, anterior hip replacement, outpatient and rapid recovery total joint replacement, patient-specific or custom implants, robotic-assisted surgery, computer navigation, infection, and fracture management. Learn more about Dr. Wright.
FAQs
Below are some frequently asked questions about arthritis, along with their answers.
What is osteoarthritis?
Osteoarthritis is the most common form of arthritis that affects the hip and knee joints. It occurs when the protective cartilage that cushions the ends of bones wears down over time, leading to pain, stiffness, and reduced joint movement.
What is rheumatoid arthritis?
Rheumatoid arthritis is an autoimmune disorder that can affect multiple joints, including the hips and knees. It occurs when the immune system mistakenly attacks the synovium, the lining of the membranes that surround the joints, leading to inflammation, pain, and eventually joint damage.
What are the symptoms of hip and knee arthritis?
Common symptoms include joint pain, stiffness, swelling, and reduced range of motion. Individuals with arthritis may also experience difficulty in walking, climbing stairs, and performing daily activities.
What are the risk factors for developing hip and knee arthritis?
Risk factors include age, family history, obesity, joint injuries, and certain occupations that involve repetitive joint movements.
How is arthritis diagnosed?
Diagnosis often involves a combination of medical history, physical examination, imaging tests (X-rays, MRI), and sometimes blood tests to rule out other forms of arthritis.
Can arthritis be prevented?
While some risk factors are beyond control, maintaining a healthy weight, staying physically active, and avoiding joint injuries can help reduce the risk of developing arthritis.
What are the treatment options for hip and knee arthritis?
Treatment may include medications (pain relievers, anti-inflammatory drugs), physical therapy, lifestyle modifications, and in some cases, surgical interventions such as joint replacement.
Are there alternative treatments for arthritis?
Some people find relief through alternative therapies like acupuncture, massage, and dietary supplements. However, it’s essential to consult with a healthcare professional before trying these approaches.
Related Articles:
- 5 Exercises for Joint Pain: Why Variety is the Key to Relief
- Missed Your Walk Today? 6 Ways to Stay Motivated and Why
- How to Overcome Exercise Excuses: Exercise and Age
Disclosure: The information in this article is not intended as medical advice. Please visit your physician if experiencing health issues.










